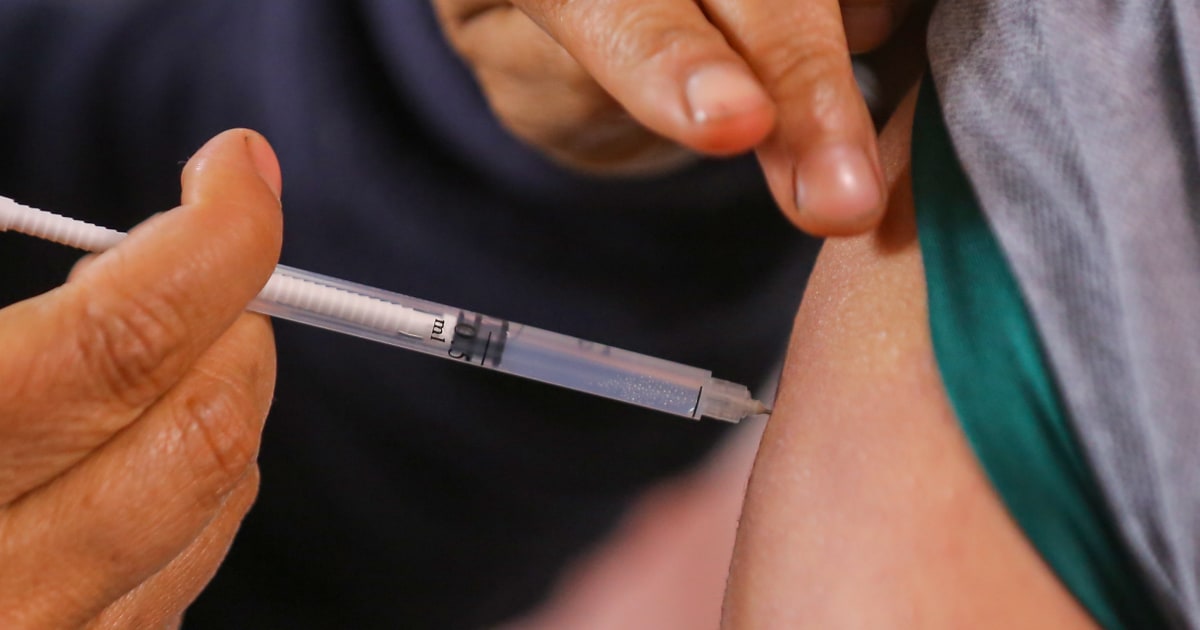
Alarming Rise: HPV-Linked Cancer Cases Surge Among U.S. Women
In recent years, the United States has witnessed a disturbing trend: an increase in cancer cases linked to the human papillomavirus (HPV) among women. This alarming rise not only poses significant public health challenges but also underscores the urgent need for greater awareness and preventive strategies. Understanding the connection between HPV and certain types of cancer is crucial for promoting health and well-being among women across the nation.
Understanding HPV and Its Link to Cancer
The human papillomavirus is a group of more than 200 related viruses, many of which are transmitted through intimate skin-to-skin contact. While most HPV infections resolve spontaneously without causing health problems, some strains are known to lead to various cancers, particularly cervical cancer. According to the Centers for Disease Control and Prevention (CDC), nearly all cases of cervical cancer can be attributed to persistent HPV infection.
In addition to cervical cancer, HPV is associated with several other types of cancer, including:
- Vulvar Cancer: This cancer affects the external female genitalia and is also linked to HPV.
- Vaginal Cancer: Similar to vulvar cancer, this type affects the vagina and has a strong association with HPV.
- Anal Cancer: Both men and women can develop anal cancer linked to HPV, but the rates are particularly concerning among women.
- Oral and Throat Cancers: Certain HPV strains, especially HPV type 16, are implicated in oropharyngeal cancers.
The Rising Statistics: A Closer Look
Recent studies have highlighted a concerning uptick in HPV-related cancer cases among women in the U.S. For instance, the American Cancer Society reports that cervical cancer incidence rates have been rising in certain demographics, particularly among women who are under-screened or have limited access to healthcare.
According to the latest data from the CDC, about 13,000 new cases of invasive cervical cancer are diagnosed annually, with an increasing proportion of these cases occurring in women aged 30 to 39. Additionally, a troubling trend has emerged, revealing that HPV-associated oropharyngeal cancers are becoming increasingly common, particularly among women, which has historically been a male-dominated issue.
Contributing Factors to the Surge
Several factors contribute to the alarming rise of HPV-linked cancer cases among U.S. women:
- Inadequate Screening: Regular Pap smears and HPV testing are crucial for early detection of cervical cancer. However, many women do not receive regular screenings due to lack of access, awareness, or healthcare coverage.
- Vaccine Uptake: The HPV vaccine is effective in preventing many HPV-related cancers. However, vaccination rates remain lower than desired, particularly among certain racial and socioeconomic groups.
- Stigma and Misinformation: Misinformation about HPV and its vaccines can deter individuals from seeking vaccination or screening. Stigmas associated with sexually transmitted infections can also prevent open discussions about HPV.
Addressing the Public Health Challenge
The surge in HPV-linked cancer cases demands a multifaceted approach to public health. Here are some critical strategies that can help combat this issue:
1. Enhancing Awareness and Education
Public health campaigns should focus on educating women about HPV, its risks, and the availability of vaccines. Effective communication can empower women to take charge of their health, seek vaccinations, and participate in regular screenings.
2. Increasing Access to Vaccination
Policy initiatives should aim to increase access to the HPV vaccine, especially in underserved communities. This includes making the vaccine available at no or low cost, as well as integrating vaccination programs into schools and community health centers.
3. Improving Screening Programs
Efforts should be made to enhance screening programs for cervical cancer and other HPV-linked cancers. This might involve mobile clinics, community outreach, and partnerships with organizations that serve vulnerable populations.
4. Engaging Healthcare Providers
Healthcare professionals should be equipped with the latest information regarding HPV and its associated cancers. Training programs and resources can help them discuss HPV vaccination and screening options with their patients more effectively.
The Role of the HPV Vaccine
The HPV vaccine is a game-changer in the fight against HPV-related cancers. Approved for both males and females, this vaccine can prevent the majority of HPV-related cancers when administered before the onset of sexual activity. Experts recommend that all preteens receive the vaccine, ideally around ages 11 to 12, although it can be given up to age 26 for females and age 21 for males.
Despite the proven efficacy of the HPV vaccine, vaccination rates remain lower than necessary. According to the CDC, only about 54% of adolescents were fully vaccinated against HPV in 2021. Increasing awareness of the vaccine’s benefits and dispelling myths surrounding it are essential for improving these rates.
Conclusion: A Call to Action
The alarming rise of HPV-linked cancer cases among U.S. women is a wake-up call for individuals, healthcare providers, and policymakers alike. By working together to raise awareness, enhance access to screenings and vaccinations, and improve education on HPV, we can combat this troubling trend.
Ultimately, the fight against HPV-related cancers is not solely about statistics; it’s about the lives of women and their families. With concerted efforts, we can hope for a future where these cancers are significantly reduced, ensuring better health outcomes for generations to come. The time for action is now, and every step we take can make a difference in the lives of women across the nation.
See more WebMD Network